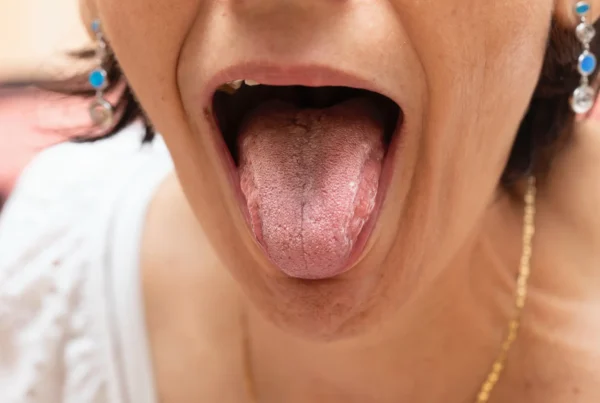In brief:
Oral thrush, also known as candidiasis, is an infection caused by yeast of the Candida genus. It most commonly presents as a white coating on the tongue, a burning sensation in the mouth, and an unpleasant taste. Although it can affect anyone, people with weakened immunity or an imbalance in oral microflora are particularly at risk. Proper oral hygiene and prompt treatment help effectively limit the development of the infection.
What is oral thrush?
Oral thrush is an infection of the mucous membrane caused by Candida yeast, which naturally occur in the human body. Under normal conditions, their levels are controlled by the immune system and the bacteria present in the oral cavity.
The problem arises when the balance of microorganisms is disrupted. In such cases, yeast can begin to multiply excessively, leading to infection. Candidiasis most commonly affects:
- the tongue,
- the palate,
- the inner sides of the cheeks,
- the gums.
In some cases, the infection may involve a larger part of the oral cavity.
Common causes of oral thrush
The development of candidiasis is often linked to a weakening of the body’s natural defense mechanisms. Several factors can increase the risk of infection, including:
- weakened immune system,
- use of antibiotics,
- diabetes,
- dry mouth,
- smoking,
- poor oral hygiene,
- long-term use of inhaled steroids.
Oral thrush, sometimes also referred to as tongue thrush, is more common in people who wear dentures – especially if they are not cleaned regularly and thoroughly.
Symptoms of oral candidiasis
Symptoms of oral thrush can vary depending on the severity of the infection. One of the most characteristic signs is a white coating on the tongue or oral mucosa. Other symptoms include:
- burning sensation of the tongue or palate,
- redness of the mucous membrane,
- unpleasant taste in the mouth,
- difficulty swallowing,
- cracks at the corners of the mouth,
- tongue sensitivity.
The coating often resembles a cottage cheese-like layer and may be partially removed, revealing a red, irritated surface underneath.
How is oral thrush treated?
Treatment of candidiasis depends on the cause and severity of symptoms. In most cases, antifungal medications are used, which may come in the form of rinses, gels, or tablets. It is equally important to eliminate factors that promote infection. This may include:
- improving oral hygiene,
- adjusting or thoroughly cleaning dentures,
- controlling blood sugar levels,
- reducing smoking.
In many cases, improving daily oral hygiene plays a key role in preventing recurrence.
Why is tongue hygiene so important?
The tongue is a place where bacteria, food debris, and microorganisms easily accumulate. If it is not cleaned regularly, it can become an environment that promotes infection.
That’s why daily oral hygiene should include not only brushing your teeth but also cleaning the surface of the tongue. This helps reduce the growth of bacteria and yeast responsible for bad breath and oral infections.
Supporting oral hygiene – Smilesonic AquaFlow irrigator
Modern oral care devices can also help maintain good oral hygiene. One example is the Smilesonic AquaFlow irrigator, which uses a pulsating stream of water to thoroughly clean interdental spaces and the gumline.
This device can also be used for gentle cleaning of the tongue surface (thanks to an additional tip included in the set), helping to remove accumulated coating and bacteria. Regular tongue hygiene can support the prevention of many oral health problems, including those related to excessive microbial growth.
Jak zapobiegać grzybicy jamy ustnej?
Profilaktyka odgrywa bardzo ważną rolę w zapobieganiu kandydozie. Najważniejsze jest utrzymanie odpowiedniej higieny jamy ustnej oraz dbanie o ogólny stan zdrowia. Warto pamiętać o kilku podstawowych zasadach:
-
- szczotkowaniu zębów co najmniej dwa razy dziennie,
-
- regularnym czyszczeniu języka,
-
- stosowaniu nici dentystycznej lub irygatora,
-
- regularnych wizytach kontrolnych u dentysty,
-
- ograniczeniu nadmiaru cukru w diecie.
Dzięki tym prostym nawykom można znacząco zmniejszyć ryzyko rozwoju infekcji w jamie ustnej.
FAQ – najczęściej zadawane pytania